- Document History
- Subscribe to RSS Feed
- Mark as New
- Mark as Read
- Bookmark
- Subscribe
- Printer Friendly Page
- Report to a Moderator
- Subscribe to RSS Feed
- Mark as New
- Mark as Read
- Bookmark
- Subscribe
- Printer Friendly Page
- Report to a Moderator
Communication for Critical Care
Patrick Ingram, Katie Maertens, Zhanpeng Zhang
Introduction:
It is the goal of our final project to create a system that allows patients with limited vocal and movement
abilities, such as individuals in the intensive care unit, to successfully communicate their needs textually and
verbally through the use of an electrooculograph (EOG). When a patient is placed in critical care, they are often
hooked to ventilation systems, IVs, and are restrained in some manner. With tubes in their throats and injured, weak,
or restrained limbs, critical care patients have great difficulty expressing their desires and communicating with those
around them. Friends, family, doctors and nurses must play guessing games with the patient. This isolation can lead
to patients feeling frustrated and depressed, and this negative state can actually hinder recovery. Allowing a means
for these patients to communicate will alleviate feelings of isolation and assist doctors in treating the individual.
Skin surface electrodes are placed around the patient’s eyes to acquire signals from the muscles controlling
the eye. The magnitude of the signal measured is linearly dependent of the angle of rotation of the eye, and as such,
if the subject distance from a viewing screen is known, the position at which the subject is looking can be
determined from vertical and horizontal EOG signals. The signal from the electrodes will be first processed though
hardware filter and gain stages to increase the SNR prior to acquisition by the on-computer DAQ. The DAQ will
provide the signal to the LabVIEW VI that will further filter and analyze the signal. The VI will be calibrated to the
individual subject’s signal amplitude and allow the software to determine which output the patient desires. This
string output will be sent to a text-to-speech sub-module for auditory output from the computer speakers.
Experimental Setup:
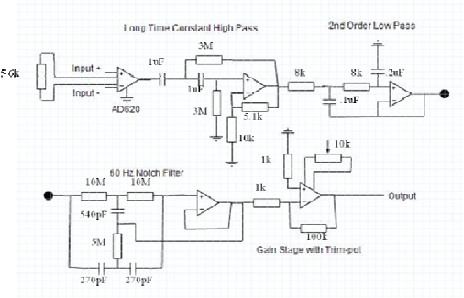
The system itself consisted of skin surface
electrodes, breadboard hardware, LabVIEW VI, and
speaker system. Gold plated electrophysiology
skin surface electrodes were purchased and taped
to the subject’s skin to help provide highest signal
fidelity from the start as it will affect all following
stages. The hardware was originally built for 1000
gain with a pass band from .5 to 200 Hz with MF741
and AD620 amplifiers. This design, however, had
significant DC offset, railing out the signal. When
the gain was reduced, the signal to noise ratio was
still insufficient to resolve the waveform. In
redesigning the hardware, a 0.08 Hz long time
constant high pass filter was added to reduce drift
but prevent recovery artifacts when the patient
returns their view to the center. The final design is
shown above and includes a differential front end with gain equal to 10, the high pass filter described above, a 2nd
order low pass filter with a cutoff of 200 Hz, a band reject filter design to attenuate 60 Hz noise and finally a gain
stage with an offset potentiometer to allow adjustment of the end stage DC offset. Overall system gain was set to
1000 (60 dB) to prevent railing on the operational amplifiers. In addition, for this design Op07, ultra low offset
amplifiers, were used to reduce drift.
These recorded signals were used to
select phrases from the front panel or choose
new tab, which contains a new subset of options.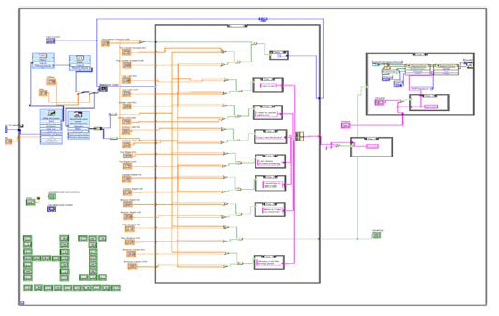
After reading the signals through the DAQ, the
software VI further conditions the signal through a
60 Hz notch filter and low pass, smoothing filter.
Digital gain and offset is then added to the signal
to ensure both left/right and up/down signals are
positive. RMS voltage values are calculated based
on a 1/10th of a second interval for each signal,
and these values were compared against set
thresholds to determine the on-screen selection. If
the on-screen selection was a new tab closed loop
feedback changes a case structure to the new
selection. Otherwise, a string for the threshold case is sent to the “output” global variable for confirmation. If the
patient blinks hard, confirming the selection, the string is processed by the text-to-speech module for auditory
output.
Results
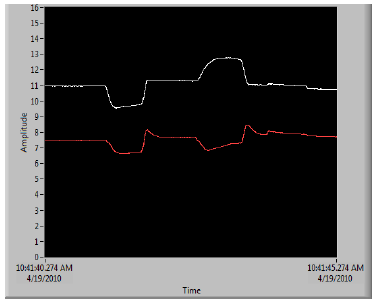
The figure below shows successful acquisition of both the left and right EOG signals from a patient into the
LabVIEW VI. For the given waveform the subject looked down and to the left and subsequently down and to the
right. Each major direction was demonstrated to have a characteristic
wave shape for the two signals taken together (up and up, down and
up, up and no change, etc), and this was used for threshold
characterization. Upon testing the system, subjects were successfully
able to hold a conversation saying on average 6 phrases per minute.
Our original acceptance criteria included communicability, speed,
accuracy, and universality. Communicability was shown in the ability
to carry out a normal conversation with another subject over a 1
minute time period. Speed was demonstrated by outputting 6 phrases
consecutively in the given time. Its accuracy was validated in the fact
that all of the phrases outputted were the ones that the patient intended
to select. Finally, the systems universality was demonstrated by
showing successful testing on two users after a recalibration. This
design is reasonably robust and reliable if calibrated properly for the
subject. While selection may sometimes take 2 tries, outputting the incorrect phrase is never an issue.
Discussion and Conclusion
The system described was tested on two individuals during multiple phases of completion. Subjects were
successful at selecting the desired phrase to respond to the questions testers posed to them. As a result, we conclude
that our system is a successful proof of concept capable of providing patients with limited mobility and vocalization
the ability to communicate with those around them. One of the major sources of error was the DC drift of the signal
due to instability and the subject naturally looking around. This could sometime even drift significantly enough to
trigger a threshold. This problem could be alleviated by the patient staying focused on the task. Additionally
electrode motion artifacts or slipping caused errors in the system. These could be addressed by acquiring higher
quality self-adhesive electrodes. Additionally, in characterizing circuit functionality through the bode plot below we
see that it does not match the proposed design specifications the complex high pass and notch filter were created
using approximate values and can contribute to the disparities with the original design.
Application
Some additional feature that we could add to our project could include the following: the capability to
personalize, ability to control media devices, output voice customization, and more ideal electrode setup. If patients
could personalize the system to what output fits their needs the system would be much more robust. Currently the
patient is limited by the phrases they can say, however, with the ability to personalize they could add in other pages
and buttons they would feel necessary. This could be implemented by displaying a new page button and a full
keyboard on the screen that would allow patients to “type” and save their new phrases. If the system was integrated
with media devices this would ease the reliability of the patient on others. Instead of having to ask someone to turn
the TV on our system would turn it on directly when that output was chosen. Also, our system could be integrated
with the nurse calling system. Typically to call a nurse there is a button near the side of the bed, however, this could
be hard to push for a person in critical care. With our system they could just select the nurse calling button on the
screen and a nurse would be sent in. This would save nurses time so that they wouldn’t have to constantly check to
see if the patient was in need of anything. Implementing this would require syncing and wiring our system with
other media systems in the hospitals. Having the ability to customize the voice would add some satisfaction with the
patients. If a male patient only had the option of using a female voice they may not feel like they are not actually
carrying on the conversation. This could be implemented by downloading more voice options from the internet and
adding them to a voice database which the patient could look through. Finally, having a more ideal electrode setup
would make the system more comfortable for the patient to wear and easier for the doctor or nurse to set up. Only
two electrodes could be use if the angle of rotation of the eye was used instead of thresholds. The electrodes could
be wireless and embedded into thin strips of a sticky material. These strips could easily be placed on a patient and
the patient would not be bothered by numerous electrodes and wires.
Attachment: Original Report
- Mark as Read
- Mark as New
- Bookmark
- Permalink
- Report to a Moderator
Hi! Can everyone share for me Labview Code of this Project? Thanks
